The Cancer Grade is the description of a tumour based on how abnormal the tumour cells and the tumour tissue look under a microscope. For more detail on Cancer Grade please refer to the section “The Gleason Score.”
The Cancer Stage refers to the size and extent of the tumour and whether or not cancer cells have spread in the body.
Staging is determined by the results of the mpMRI, the biopsy, and the histopathology report when the biopsy samples are examined.
Staging for Prostate Cancer can also require other scans (beyond the mpMRI scan) to determine if the cancer has metasticised – has spread from the prostate to other parts of the body. Knowing the Stage helps to determine what kind of treatments are appropriate and can help predict a patient’s prognosis (the chance of recovery). There are different Stage descriptions for different types of cancer – 2 types of Staging are used for Prostate Cancer:
Clinical Staging: this is based on the results of direct rectal examination, PSA testing, and most importantly, the Gleason score. These test results will help determine whether X-Rays, Bone scans, PET scans, Whole Body – Diffusion Weighted MRI scans, and/or CT scans are also required.
Pathologic Staging: this is based on information found if surgery is performed, plus the laboratory results, of the prostate tissue removed by biopsy or during surgery. If surgery includes the removal of the entire prostate, then some lymph nodes will also be removed. Examination of the removed lymph nodes can provide more information for pathologic staging especially to indicate if the cancer might have metasticised.
The TNM Staging system
One tool that doctors use to describe the Stage is the TNM system. The results from diagnostic tests and scans are used to answer the following questions:
- Tumour (T): How large is the primary tumour ? Where is it located ?
- Node (N): Has the tumour spread to the lymph nodes? If so, where, and how many ?
- Metastasis (M): Has the cancer metastasized to other parts of the body? If so, where and how much?
The results are combined to determine the stage of cancer. There are 5 stages: stage 0 (zero) and stages I to IV. The stage provides a common way of describing the cancer and potential treatment options considered.
Tumour (T)
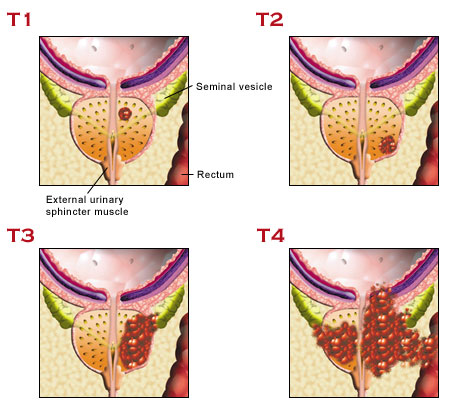
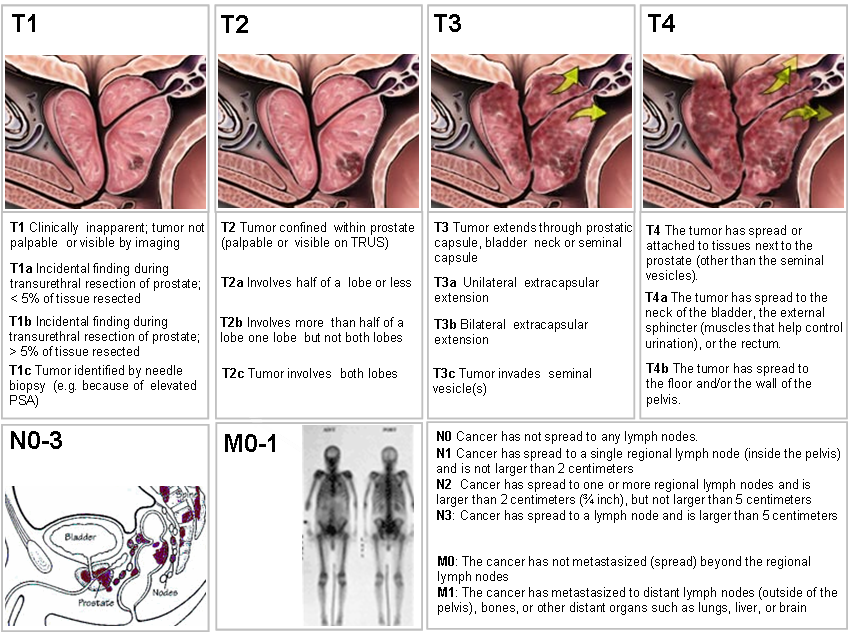
Using the TNM system, the “T” plus a letter or number (0 to 4) is used to describe the size and location of the tumour. Some stages are also divided into smaller groups that help describe the tumour in even more detail. Specific tumour stage information is listed below. If the tumour is staged clinically, it is often written as cT. If pathologic staging is used, it is written as pT.
Clinical T
- TX: The primary tumour cannot be evaluated.
- T0 (T plus zero): There is no evidence of a tumour in the prostate.
- T1: The tumour cannot be felt during a DRE and is not seen during imaging tests. It may be found when surgery is done for another reason, usually for BPH or an abnormal growth of noncancerous prostate cells.
- T1a: The tumor is in 5% or less of the prostate tissue removed during surgery.
- T1b: The tumour is in more than 5% of the prostate tissue removed during surgery.
- T1c: The tumour is found during biopsy.
- T2: The tumour is found only in the prostate, not other parts of the body. It is large enough to be felt during a DRE.
- T2a: The tumour involves one-half of 1 side of the prostate.
- T2b: The tumour involves more than one-half of 1 side of the prostate but not both sides.
- T2c: The tumour has grown into both sides of the prostate.
- T3: The tumour has grown through the prostate on 1 side and into the tissue just outside the prostate.
- T3a: The tumour has grown through the prostate either on 1 or both sides of the prostate. This is called extraprostatic extension (EPE).
- T3b: The tumour has grown into the seminal vesicle(s), the tube(s) that carry semen.
- T4: The tumour is fixed, or it is growing into nearby structures other than the seminal vesicles, such as the external sphincter, the part of the muscle layer that helps to control urination; the rectum; the bladder; levator muscles; or the pelvic wall.
Pathological T
There is no TX, T0, or T1 classification for pathologic staging of prostate cancer.
- T2: The tumour is found only in the prostate.
- T3: There is EPE. The tumour has grown through the prostate on 1 or both sides of the prostate.
- T3a: There is EPE or the tumour has invaded the neck of the bladder.
- T3b: The tumour has grown into the seminal vesicle(s).
- T4: The tumour is fixed, or it is growing into nearby structures other than the seminal vesicles, such as the external sphincter; the rectum; the bladder; levator muscles; or the pelvic wall.
Node (N)
The “N” in the TNM staging system stands for lymph nodes. These tiny, bean-shaped organs help fight infection. Lymph nodes near the prostate in the pelvic region are called regional lymph nodes. Lymph nodes in other parts of the body are called distant lymph nodes. Lymph nodes are often the ‘transport’ mechanism whereby cancer cells spread around the the body and metasticise.
- NX: The regional lymph nodes cannot be evaluated.
- N0 (N plus zero): The cancer has not spread to the regional lymph nodes.
- N1: The cancer has spread to the regional (pelvic) lymph node(s).
The “M” in the TNM system indicates whether the prostate cancer has spread to other parts of the body, such as the lungs or the bones. This is called distant metastasis.
- MX: Distant metastasis cannot be evaluated.
- M0 (M plus zero): The disease has not metastasized.
- M1: There is distant metastasis.
- M1a: The cancer has spread to distant, lymph node(s).
- M1b: The cancer has spread to the bones.
- M1c: The cancer has spread to another part of the body, with or without spread to the bone
 Used with permission of the American College of Surgeons, Chicago, Illinois. The original and primary source for this information is the AJCC Cancer Staging Manual, Eighth Edition (2017), published by Springer International Publishing.
Used with permission of the American College of Surgeons, Chicago, Illinois. The original and primary source for this information is the AJCC Cancer Staging Manual, Eighth Edition (2017), published by Springer International Publishing.
Cancer Stage Grouping
Doctors assign the Stage of the cancer by combining the T, N, and M classifications. Staging also includes the PSA level and Grade Group.
Stage I: Cancer in this early stage is usually slow growing. The tumour cannot be felt and involves one-half of 1 side of the prostate or even less than that. PSA levels are low. The cancer cells are well differentiated, meaning they look like healthy cells (cT1a–cT1c or cT2a or pT2, N0, M0, PSA level is less than 10, Grade Group 1).
Stage II: The tumour is found only in the prostate. PSA levels are medium or low. Stage II prostate cancer is small but may have an increasing risk of growing and spreading.
Stage IIA: The tumour cannot be felt and involves half of 1 side of the prostate or even less than that. PSA levels are medium, and the cancer cells are well differentiated (cT1a–cT1c or cT2a, N0, M0, PSA level is between 10 and 20, Grade Group 1). This stage also includes larger tumours confined to the prostate as long as the cancer cells are still well differentiated (cT2b–cT2c, N0, M0, PSA level is less than 20, Group 1).
Stage IIB: The tumour is found only inside the prostate, and it may be large enough to be felt during DRE. The PSA level is medium. The cancer cells are moderately differentiated (T1–T2, N0, M0, PSA level less than 20, Grade Group 2).
Stage IIC: The tumour is found only inside the prostate, and it may be large enough to be felt during DRE. The PSA level is medium. The cancer cells may be moderately or poorly differentiated (T1–T2, N0, M0, PSA level is less than 20, Grade Group 3–4).
Stage III: PSA levels are high, the tumour is growing, or the cancer is high grade. These all indicate a locally advanced cancer that is likely to grow and spread.
Stage IIIA: The cancer has spread beyond the outer layer of the prostate into nearby tissues. It may also have spread to the seminal vesicles. The PSA level is high. (T1–T2, N0, M0, PSA level is 20 or more, Grade Group 1–4).
Stage IIIB: The tumour has grown outside the prostate gland and may have invaded nearby structures, such as the bladder or rectum (T3–T4, N0, M0, any PSA, Grade Group 1–4).
Stage IIIC: The cancer cells across the tumour are poorly differentiated, meaning they look very different from healthy cells (any T, N0, M0, any PSA, Grade Group 5).
Stage IV: The cancer has spread beyond the prostate.
Stage IVA: The cancer has spread to the regional lymph nodes (any T, N1, M0, any PSA, any Grade Group).
Stage IVB: The cancer has spread to distant lymph nodes, other parts of the body, or to the bones (any T, N0, M1, any PSA, any Grade Group).
Recurrent: Recurrent Prostate Cancer is cancer that has come back after treatment. It may come back in the prostate area again or in other parts of the body. If the cancer does return, there will be another round of tests to learn about the extent of the recurrence. These tests and scans are often similar to those done at the time of the original diagnosis.

 Used with permission of the American College of Surgeons, Chicago, Illinois. The original and primary source for this information is the AJCC Cancer Staging Manual, Eighth Edition (2017), published by Springer International Publishing.
Used with permission of the American College of Surgeons, Chicago, Illinois. The original and primary source for this information is the AJCC Cancer Staging Manual, Eighth Edition (2017), published by Springer International Publishing.